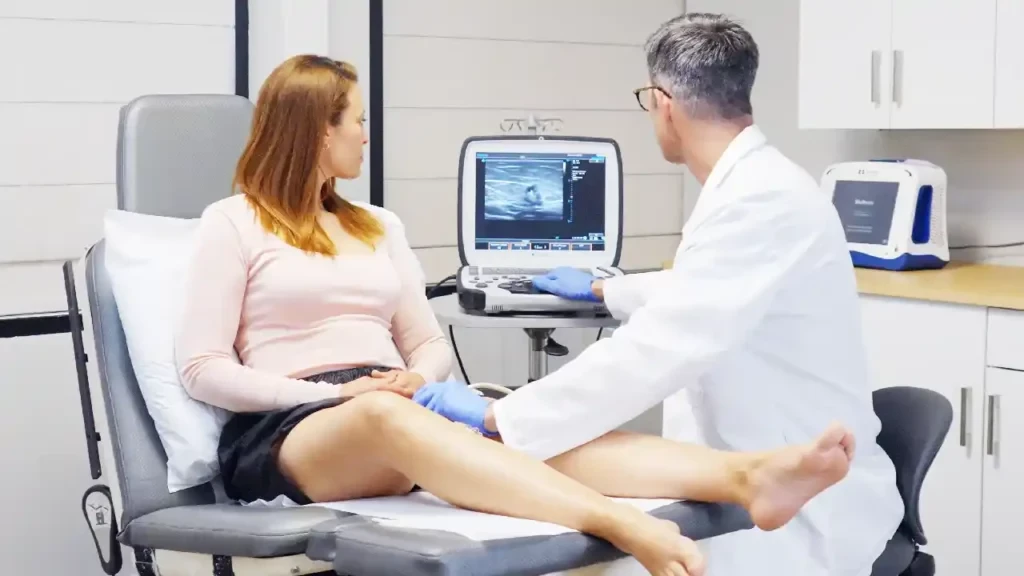
Do You Have Chronic Venous Insufficiency (Photos)?
Have you been diagnosed with chronic venous insufficiency (CVI)? Or do you have spider veins, varicose veins, edema, or other symptoms that suggest you have the disease? Click HERE to see chronic venous insufficiency photos, and more importantly, book an appointment for an expert’s diagnosis at our award-winning California vein center.
Successfully treating surface veins like varicosities and telangiectasias often involves treating underlying issues like CVI. So, what is the best treatment for venous insufficiency? The answer depends on your unique medical history and symptoms, but the great news is most patients only require minimally invasive procedures that are completed in minutes at our state-of-the-art vein centers in California.
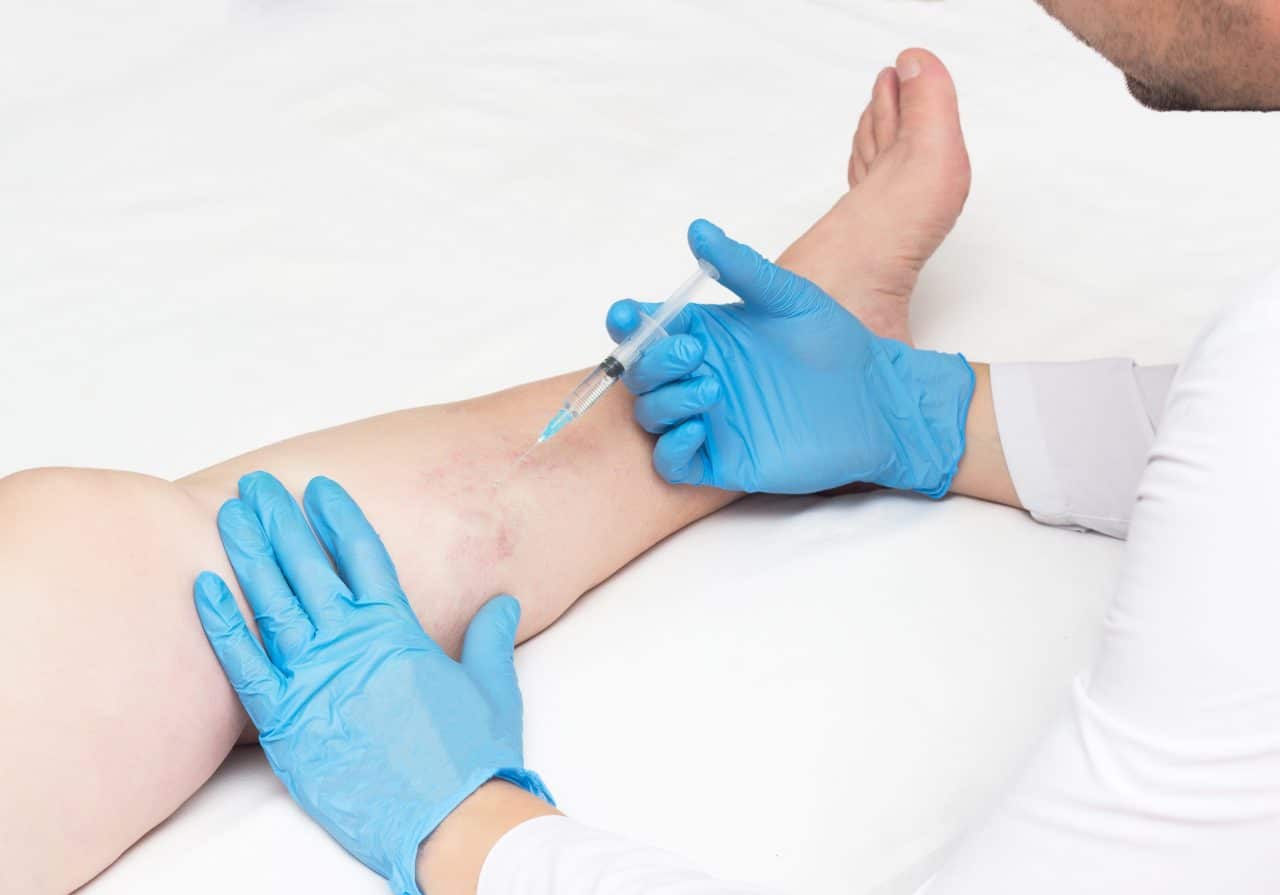
What Are the Most Common Femoral Vein Reflux Treatments?
There are several minimally invasive procedures for CVI. The most common femoral vein reflux treatments and saphenous vein treatments include sclerotherapy, radiofrequency ablation, endovenous laser ablation, vein adhesives, and mechanochemical ablation. These are all administered without general anesthesia or large incisions, so they’re performed in our vein center without the need for hospitalization or recovery time.
Our CA vein specialists use duplex ultrasound to locate the origin of malfunction, which is typically broken valves in your veins, and they use ultrasound guidance to position the treatment device at the source. By doing so, they close off malfunctioning valves so that blood will no longer pool in the veins and create spider veins and varicose veins. They also improve blood flow by eliminating unhealthy veins and redirecting blood into healthier veins.
While this requires great skill and precision from the vein doctor, it is easy for the patient, and they are able to move about immediately after the procedure and resume their regular activities. Most of the common femoral vein reflux treatments are minimally invasive procedures that utilize tiny needles or catheters to deliver medicine, thermal energy, or cyanoacrylate glue to the vein’s walls. These are all quick and gentle procedures that require no downtime for the patient.
What’s the Best Deep Vein Insufficiency Treatment?
It’s important to note that successfully eliminating the damaged veins you see at the surface requires looking for trouble in deeper veins. Chronic venous insufficiency is a condition that involves broken valves in your veins found deeper in the leg. You can’t see that malfunction from the surface, but it’s what causes blood to pool and generate the enlarged, bulging, or spidery veins you see beneath your skin. If you don’t address the deeper issue, surface vein damage will continue to appear.
Deep vein insufficiency treatment requires a qualified vein specialist, like our Harvard-trained vein doctors in California, who use duplex ultrasound to examine your entire venous anatomy. Some vein centers only treat the superficial damage, but that won’t permanently resolve the problem. Surface lasers and sclerotherapy for surface veins won’t correct deep vein insufficiency. This requires endovenous procedures that target the valve malfunction behind venous reflux. Visit our fully accredited, cutting-edge vein centers in California for comprehensive vein care.
Does Saphenous Vein Reflux Treatment Resolve CVI?
Some veins, like broken capillaries on the face, might respond to surface treatments like pulsed-dye lasers. But varicose veins, broken capillaries on legs, and saphenous vein reflux treatment typically requires treating venous insufficiency as well. Not all vein reflux treatments address CVI. Treating vein disease requires a specialist who’s trained in ultrasound imaging and minimally invasive procedures that look beyond the surface damage.
While you can treat certain spider veins with a surface laser, you can’t prevent a recurrence of spider veins, varicose veins, or venous reflux without addressing underlying venous insufficiency with endovenous methods. Our innovative vein treatments repair visible damage, as well as underlying issues, often in a single appointment. Since our vein specialists are board certified in venous medicine, they offer the latest minimally invasive procedures that provide comprehensive care in a fraction of the time.
What Kind of Doctor Treats Venous Insufficiency?
Wondering what kind of doctor treats venous insufficiency? Choose your vein specialist wisely, since some vein centers only offer surface treatments, and others only offer surgical methods. The best kind of doctor to treat venous insufficiency is a board certified vein doctor who specializes in non-surgical, minimally invasive procedures for veins.
Most patients no longer require surgery, but many patients do require more than a topical treatment for their veins. Minimally invasive vein specialists use injectable medicines or adhesives, targeted radiofrequency or lasers, or mechanical ablation to treat veins. These tactics address deeper issues without the use of invasive surgery.
Do CVI Treatments Heal Varicose Veins, Edema & Symptoms?
The best CVI treatments address the disease and also eliminate spider veins, varicose veins, edema, pain, venous ulcers, venous stasis dermatitis, and all of the unpleasant symptoms of venous insufficiency. By closing off broken valves in your veins, deoxygenated blood is rerouted into viable pathways and pumped efficiently back to the heart. Symptoms of CVI can range from uncomfortable to disabling, or even life-threatening. Our vein doctors offer rapid relief for everything from venous stasis ulcers to painful, bulging varicose veins.
Are Broken Capillaries on Legs Repaired by CVI Treatment?
Some types of vein damage don’t require endovenous CVI treatment. For instance, broken capillaries on the face often result from sun damage or skin injury. But broken capillaries on legs are more indicative of CVI, since leg veins work against gravity to pump deoxygenated blood up to the heart and are more prone to valve failure, which allows blood to pool in the veins. If you have varicose veins or broken capillaries on the legs, or concurrent symptoms like leg heaviness, venous ulcers, venous stasis dermatitis, hyperpigmentation, or edema, book an appointment today for prompt relief.
Collapsed Vein Treatments vs. How to Treat a Collapsed Vein?
Veins can collapse unintentionally, for instance, when a needle is inserted improperly, or with IV drug use, or even with aging. This usually doesn’t require treatment, but it can cause pain, discoloration, or swelling. In some cases, the vein is permanently closed and blood bypasses that vein to complete the circulation process.
In contrast, some veins are collapsed intentionally, in order to treat varicose veins or venous insufficiency. In these procedures, doctors insert a treatment like a sclerosing solution or a tiny fiber that delivers thermal energy to the vein’s walls, causing it to collapse. This prompts blood to flow away from the damaged vein and into a vein that can pump it back to the heart.
When a doctor intentionally collapses a vein, it is typically painless and rarely causes permanent discoloration, since doctors use numbing agents, ultrasound guidance, and tiny needles or catheters. Medically collapsing a vein causes it to be harmlessly absorbed by the body, rendering varicose veins and spider veins less visible.
Varicose Vein, Insufficiency, Burst Vein: Are They the Same?
A varicose vein, insufficiency, and a burst vein share some similarities, but they aren’t synonymous. Venous insufficiency is a disease that involves weakened or broken valves in the veins. This causes venous reflux (blood flowing in reverse and pooling in the vein). A common result of venous reflux is a varicose vein, which is a vein that becomes enlarged and twisted from elevated pressure in the vein.
Venous insufficiency and varicose veins are closely linked, but you might have venous insufficiency with spider veins (a new, smaller vein that branches out from an overburdened vein) rather than varicose veins, and you might also have asymptomatic CVI, so check with your vein doctor if you suspect vein issues, or if they run in your family.
The terms varicose vein and burst vein are sometimes used interchangeably, but these are not identical. A varicose vein is stretched, but a ruptured vein is one that bursts open, typically due to improper needle insertion or injury, and this can occur whether it is varicose or not. However, if a varicose vein ruptures, for instance with an abrasion to the skin above it, the bleeding can be hard to control. Seek prompt medical attention for a burst or lacerated varicose vein.
Varicose Veins Stage 1: When Should You Treat Insufficiency?
The best time to treat venous insufficiency is as soon as you suspect it. While varicose veins have stages of severity, individuals progress through the stages at different rates, and it’s impossible to predict how severe your vein damage will get. Venous insufficiency is often chronic, and it will continue to produce vein damage until it’s addressed. Simply treating the existing surface veins is only a temporary solution if you have underlying vein disease.
Consult our vein doctors for venous insufficiency and varicose veins in stage 1 to prevent unnecessary complications like venous ulcers, venous stasis dermatitis, edema, and hyperpigmentation. Regular exercise, weight loss, and jobs where you don’t sit or stand for long periods might help circulation. But only a vein doctor can repair vein disease and existing vein damage. Call us to inquire about what is the best treatment for venous insufficiency. We offer a full range of minimally invasive procedures to address every vascular need.