How Serious Are Varicose Vein Surgeries Like Phlebectomies?
History traces vein surgeries back to Hippocrates 2400 years ago. The procedure has evolved significantly, so how serious is varicose vein surgery now? The latest varicose vein surgeries include phlebectomy and ambulatory phlebectomy, which involve extracting the vein, or a portion of the vein, from the body. Traditional phlebectomies use anesthesia and multiple incisions, while ambulatory phlebectomies use smaller punctures and no anesthesia. Doctors are continually perfecting the procedures, but vascular surgeries aren’t without risk. Book an appointment with a Harvard-trained vein doctor in California to minimize these risks.
Do New Surgeries Use a Small Cut or Large Incision?
The size of the incisions and severity of the procedure depend on several factors. Vein doctors will assess your vasculature, symptoms, and medical history to select the best method. Some patients will need general or spinal anesthesia and deep incisions in the groin, knee, and calf area. Others will receive a series of small cuts or punctures through which the doctor accesses the vein. Some surgeries require a stay in the hospital and recovery time away from work. Ambulatory phlebectomy is a less invasive surgery that doesn’t employ general anesthesia. However, some veins can’t be treated with this procedure, so ask your vein specialist if you qualify.

Is Vein Surgery the Safest Way to Treat Varicose Veins?
For most patients, minimally invasive vein treatments are safer than vein surgery. Vein doctors can now treat veins inside the body, rather than surgically removing them. They insert hollow needles or thin tubes through the skin to position treatment directly on the vein’s walls. They can deliver sclerosants, thermal energy, or adhesives through these tiny tubes. These vein treatments close the vein off, so it shrinks and disappears.
Blood is then rerouted into veins that are capable of pumping it back to the heart. Minimally invasive varicose vein treatments are quicker, gentler, and easier on the patient. There is no need for general anesthesia, incisions, stitches, or hospitalization. The patient can typically drive themselves home and even go right back to work.
However, for a small percentage of patients, varicose vein surgery is the safer choice. Patients with blood clots, severe tortuosity, or other medical conditions might require surgery. Some minimally invasive procedures inject a sclerosing solution or cyanoacrylate glue into the vein which could cause a blood clot to travel. That’s why it’s important to choose a board certified vein doctor in California, not a cosmetic vein center.
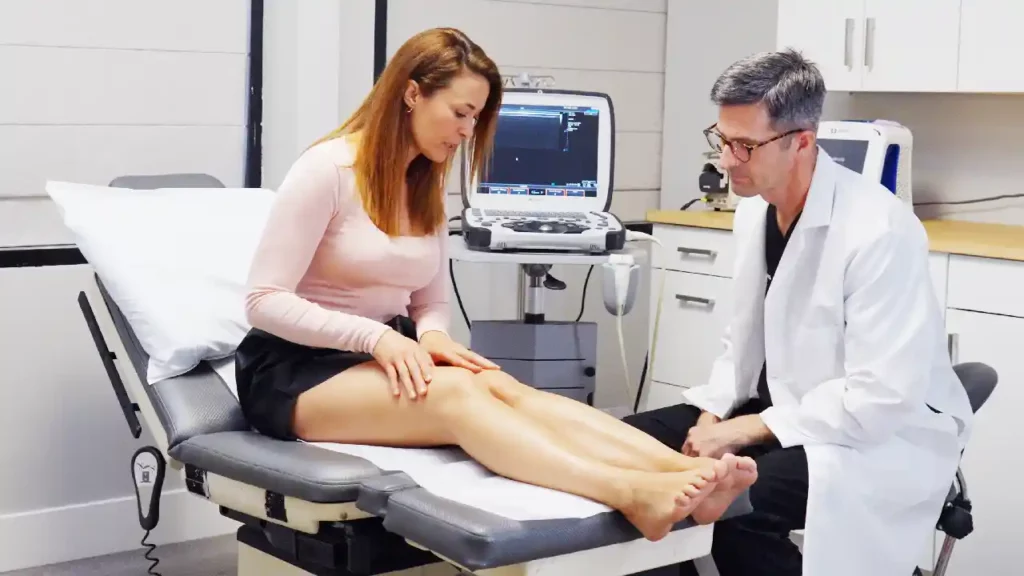
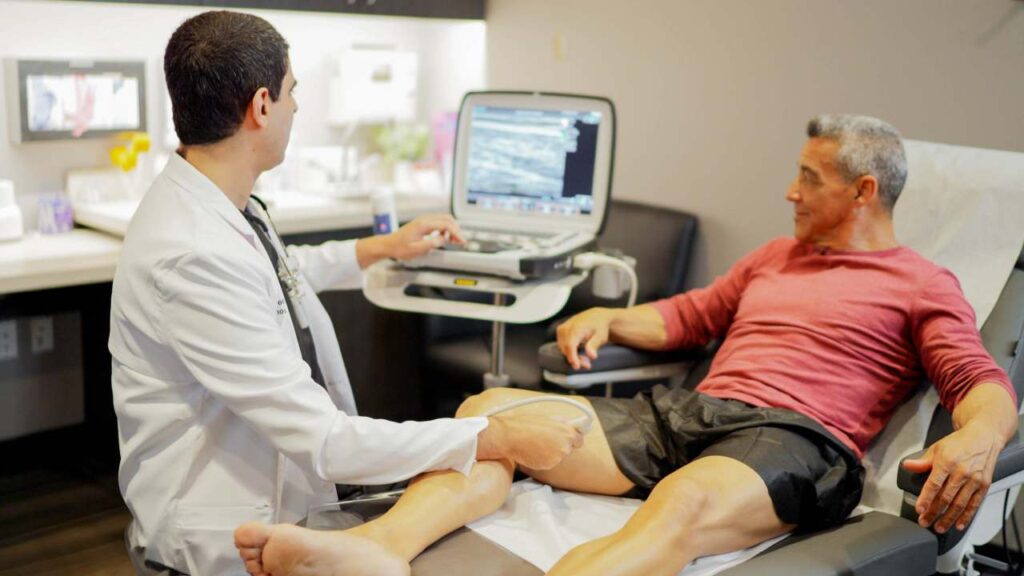
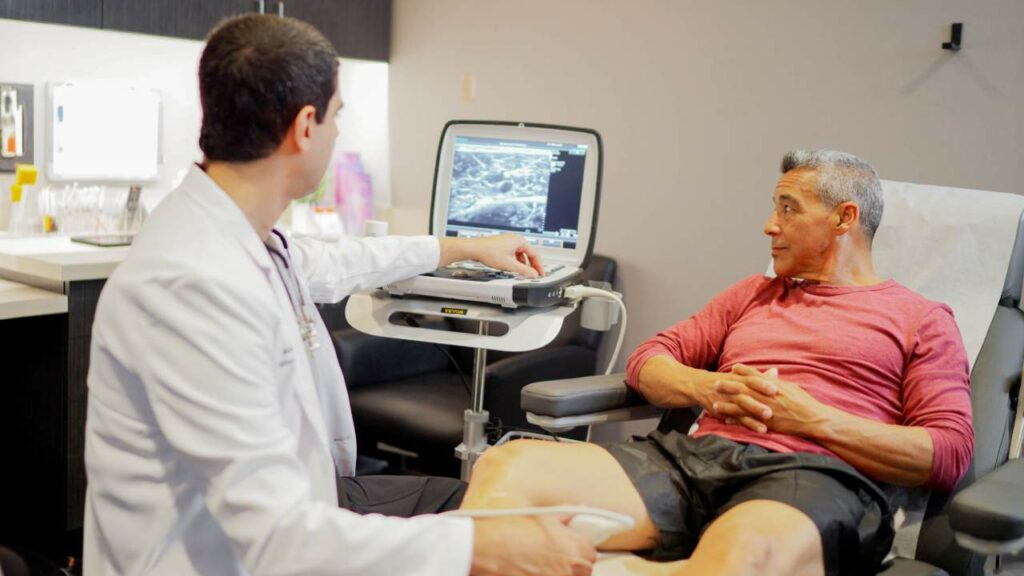
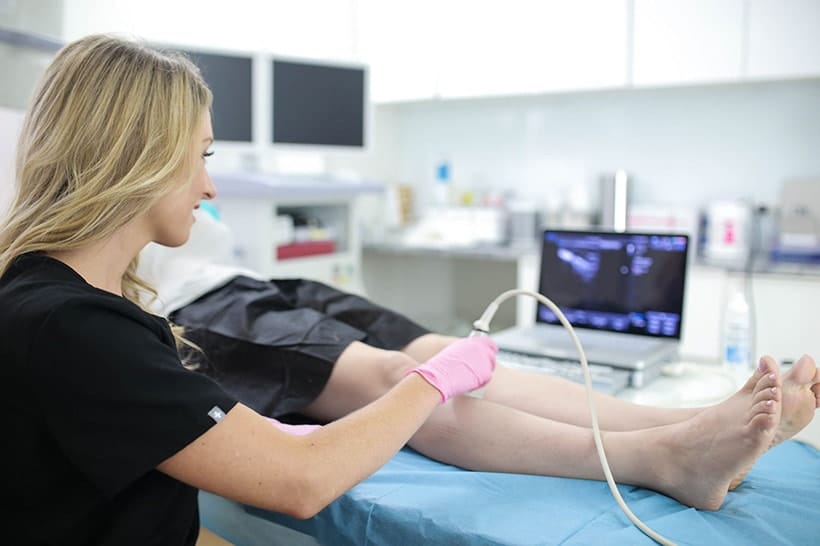
Qualified vein specialists will use Duplex Ultrasound imaging to locate blood clots and connecting veins before recommending a procedure. They’ll also use ultrasound guidance while administering vein treatment to ensure a safe and successful outcome. Our vein experts treat varicose veins with remarkable care and precision.
Are Endovenous Lasers or Radiofrequency Safer Than Surgery?
Endovenous procedures have largely replaced vein surgery. Doctors can heat veins with either lasers or radiofrequency, creating scar tissue that seals them shut. This is done with tiny needles with a fiber tip. Vein doctors insert a thin tube through your skin and inject tumescent anesthesia to surround the vein. This protects adjacent tissue from the heat. Then they activate the thermal device to cauterize the vein.
The procedure is safe and painless for most patients, and it works quickly to erase the varicose vein. Patients who are allergic to tumescent anesthesia might be advised to use a different procedure, like sclerotherapy. But the majority of patients are better suited to endovenous laser ablation or radiofrequency ablation than vein surgery.
When Should You Talk with Your Doctor About Surgery?
The sooner you talk with your doctor about varicose vein surgery, the better your outcome will be. If you are nervous about surgery, bear in mind that most patients don’t need it. For those who do need it, the technology has advanced tremendously in the last 30 years. Many patients now have ambulatory phlebectomy with minimal discomfort and recovery time.
When varicose veins go untreated, preventable complications ensue. Patients can develop cramping, swelling, restlessness, heaviness, and itching in their legs. They might also contend with venous ulcerations, hyperpigmentation, profuse bleeding, and venous stasis dermatitis. With the right vein doctor, varicose vein treatment takes less than 30 minutes, and it’s a low-risk, high-reward procedure. Schedule your consultation with our California vein specialists to prevent complications of delaying vein treatment.
Can You Just Wear Compression Stockings for Enlarged Veins?
Some patients ask whether they can just wear compression stockings rather than treating enlarged veins. For most patients, this is not an effective solution. The great saphenous vein runs the length of the leg, and it’s lined with one-way valves. When valves fail, blood flows in reverse and collects in the vein, causing those enlarged saphenous veins you see at the surface. If you wear compression stockings, the pressure might help push blood out of those defective veins.
But compression stockings won’t fix broken valves or correct the associated disease called Chronic Venous Insufficiency. At best, most patients notice less cramping or swelling when they wear compression stockings. But some patients see no improvement. In addition, patients who have venous ulcerations, venous stasis dermatitis, or blood clots may not be able to wear compression stockings.
Visit our state-of-the-art vein centers in California to see if compression therapy is right for you. If you are approved for compression stockings, our vein doctors will fit you with the right ones. The better solution is often to treat the vein with a minimally invasive procedure, rather than wearing compression stockings indefinitely. If you’re wondering, “How serious is varicose vein surgery,” the answer is you’re in good hands with a board certified vein doctor. But most patients can select a minimally invasive procedure instead of surgery.