1. Vein Pain Can Signify a Deep Vein Thrombosis
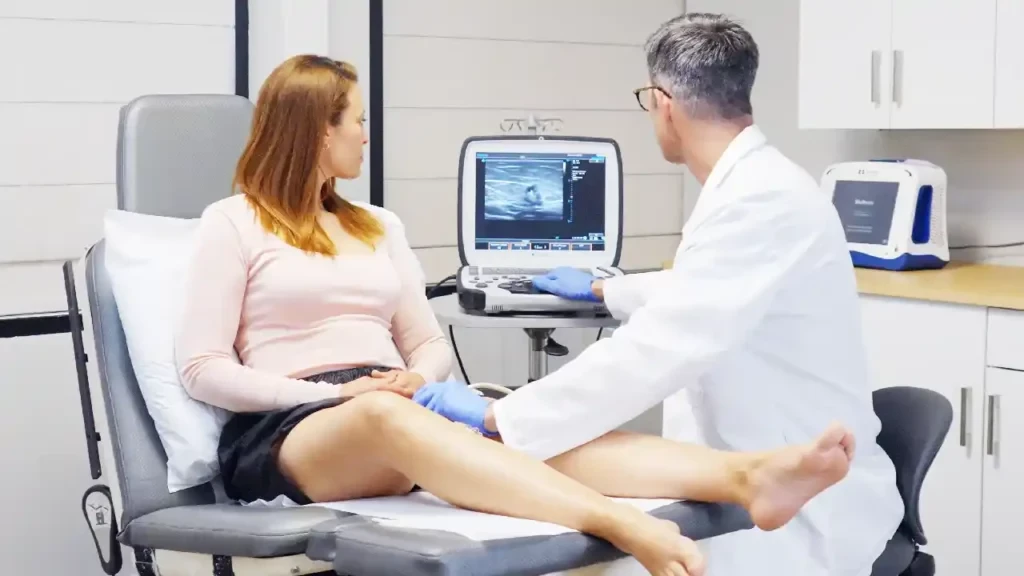
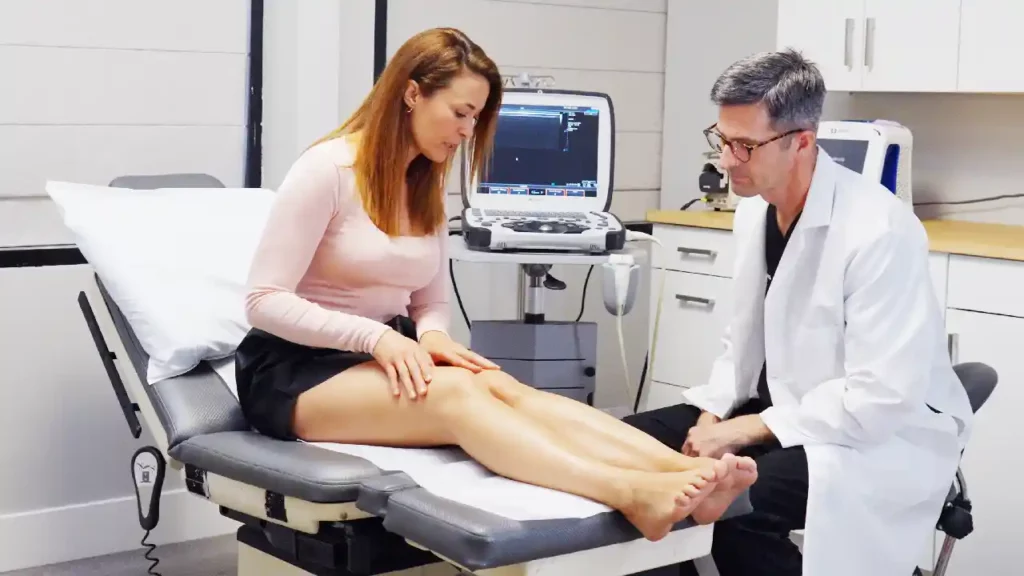
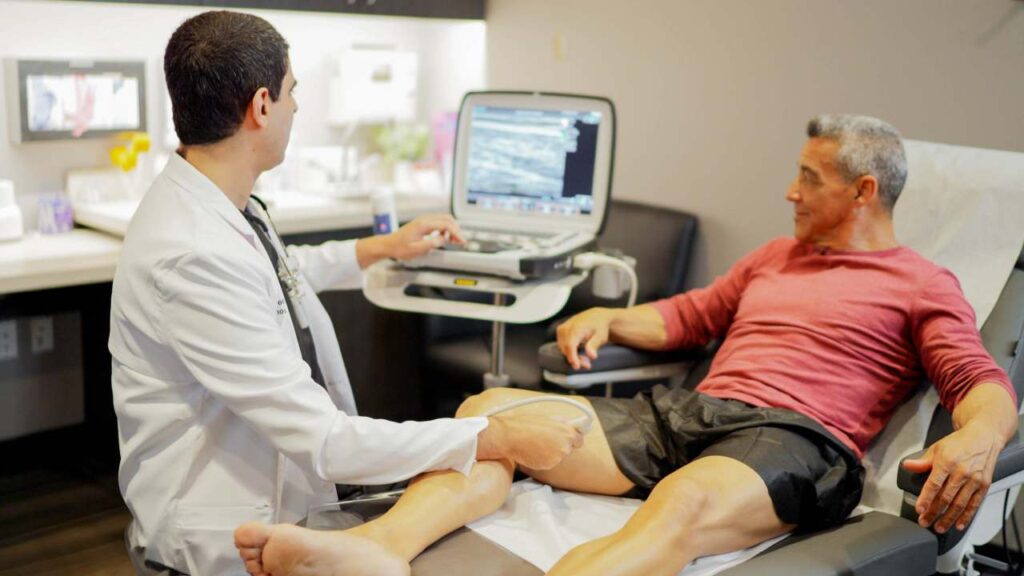
If you’re wondering, “Should I be worried if my veins hurt,” the answer is that you should see a vein doctor promptly to determine the level of concern. Some causes only require lifestyle adjustments, while others are life-threatening. The most important reason to see a vein doctor is because vein pain can signify a deep vein thrombosis (DVT). These are blood clots in deeper veins that obstruct blood flow and can be deadly if they break loose. If your vein develops a sudden raised area with redness, warmth, and pain, seek immediate medical care. If you’d like to learn more about DVTs and determine whether you have any blood clots, book an appointment with our Harvard-trained vein doctors in California. We offer comprehensive vein mapping tests to locate existing clots and prevent complications of DVTs.
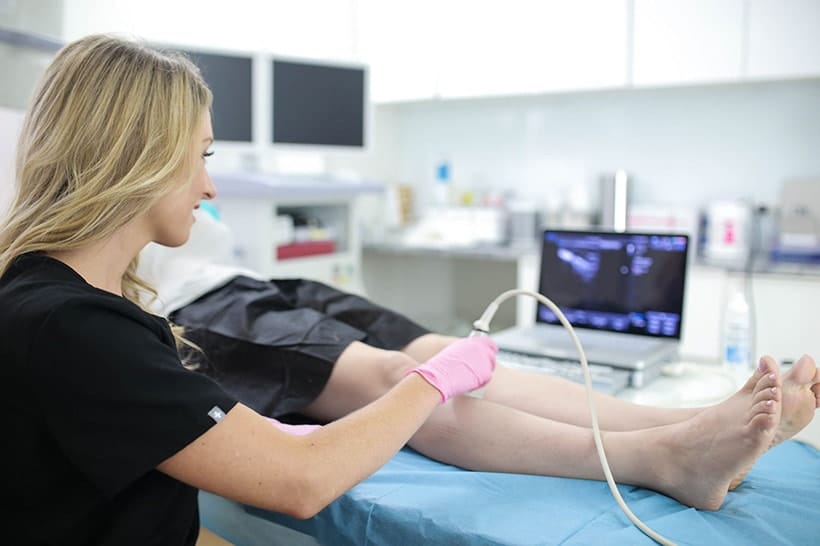 .
.
2. Blood Clots in Veins Can Cause Pulmonary Embolisms
If a DVT travels through the vein, it can block blood flow to an essential artery in the lung. This is called a pulmonary embolism. Visit a board certified vein doctor at the first sign of vein pain to prevent this outcome. If you develop chest pain, shortness of breath, lightheadedness, heart palpitations, a dry cough, or a cough that produces blood, go to the emergency room. The best way to prevent pulmonary embolisms is to be proactive about your vascular health. Our vein doctors can identify clots and treat them with measures that won’t move a DVT toward the lung. It’s important to choose a qualified vein specialist since some treatments, like blood thinners, can be dangerous for clots in certain locations.
3. Vein Pain Often Indicates Chronic Venous Insufficiency
The most common reason people develop uncomfortable veins is a condition called Chronic Venous Insufficiency (CVI). This involves weak or malfunctioning valves inside the veins that allow blood to flow in reverse. Backward blood flow causes an accumulation of blood that elevates pressure in the vein. Symptoms include leg pain, swelling, heaviness, cramping, restlessness, and fatigue. As Chronic Venous Insufficiency progresses, venous ulcerations, hyperpigmentation, and venous stasis dermatitis can develop. Minimally invasive vein treatments are the best way to treat CVI and the correlated vein pain. Treating CVI promptly helps prevent those painful complications.
4. Excess Venous Blood Pressure Can Cause Varicose Veins
Excess blood pressure from CVI can cause veins to become varicose. Varicose veins are swollen, twisted, protuberant blood vessels that are often visible through the skin. They can develop anywhere, but they’re common in leg veins, since these veins pump blood against gravity, increasing the incidence of backward blood flow. Varicose veins often cause cramping, burning, stinging, and other symptoms concurrent with CVI. It’s important to treat symptomatic varicose veins, not only for your vascular health, but also to improve how you feel.
5. Leg Pain Can Result from Spider Veins
Spider veins are another type of damaged blood vessel that result from elevated endovenous blood pressure. These are smaller and less protrusive than varicose veins, but they can cause the same symptoms. Varicose veins swell to contain excess blood, whereas spider veins are new offshoots from overburdened veins. If you have spider veins or varicose veins in your legs, you probably have CVI. See a vein doctor to assess your vascular health and discuss your vein treatment options. Our California vein centers treat spider veins, varicose veins, and CVI with quick, non-surgical, outpatient procedures.
6. Damaged Blood Vessels Can Cause Painful Skin Conditions
What happens if you don’t treat spider veins, varicose veins, or CVI? The painful symptoms can extend beyond the vein to the surface of the skin. Slow-healing venous ulcerations can form on the skin and become infected. Rust-colored discoloration can spread on the legs and feet and be difficult to reverse. Venous stasis dermatitis, or venous eczema, can produce itchy, scaly, red skin. These are all in addition to the painful symptoms inside the legs. Seeking vein treatment at the first sign of vein damage can prevent these extra sources of discomfort.
7. Peripheral Artery Disease (PAD) Can Cause Pain
It’s a common misconception that arteries and veins are synonymous. They’re both blood vessels, but they have different structures and tasks. Arteries pump oxygenated blood away from the heart. Veins pump blood back to the heart to collect more oxygen. Arteries don’t have valves, so blood can’t flow backward through them and make them varicose. But, arteries can become blocked or narrowed by conditions like peripheral artery disease (PAD). When arteries are inhibited, limbs don’t receive enough oxygen. If you have leg pain, you need to check for both venous and arterial issues.
8. Damaged Valves Inhibit Flow of Blood Back to the Heart
Veins with faulty valves don’t pump blood back to the heart efficiently. Spider veins are essentially dead-ends. They contain excess blood to offset the pressure in an engorged vein, and they don’t lead back to the heart. Varicose veins experience venous reflux, rather than a continual flow of blood in the right direction. Addressing vein pain caused by damaged valves restores efficient circulation. This improves vascular health and eliminates painful symptoms.
9. Standing for Long Periods Worsens Vascular Conditions
Another reason to see a vein doctor for vein pain is to learn whether your lifestyle is making things worse. Patients whose jobs require sitting or standing for long periods might notice their legs hurt more as the day progresses. That’s because leg muscle contractions help pump blood back to the heart. When you remain in a stationary or sedentary position, you not only have gravity working against you, but you also reduce the number of muscle contractions. So, blood begins pooling in the vein. Vein doctors might recommend a minimally invasive vein treatment. Or they might suggest lifestyle adjustments, like exercising, elevating your legs while at rest, or wearing compression stockings, depending on the severity of your condition.
10. Painful Veins Reduce Your Quality of Life
Treating vein pain isn’t just about correcting your vascular condition. It’s also about restoring your quality of life. Many people don’t realize how many symptoms are caused by unhealthy veins. Our patients are thrilled to see their energy, sleep, productivity, and outlook improve after treating their veins. Feeling tired, swollen, and sore isn’t easy to manage on a daily basis. Not to mention, visible vein damage can affect your self-esteem. If you’re debating, “Should I be worried if my veins hurt,” visit our award-winning California vein centers. Our vein specialists administer relief within minutes.
Don’t ignore your symptoms
At Vein Treatment Clinic, we’ve got California fully covered with expert vein doctors and convenient clinics across the state.
Whether you’re in Huntington Beach, Irvine, National City, Newport Beach, Palo Alto, Poway, San Diego, San Jose, or Temecula, you’ll find advanced care at one of our clinics close to home.
Patients trust our Ivy League–trained, board-certified specialists for minimally invasive treatments that improve circulation, relieve pain, and restore confidence. In California, our team includes Dr. Farshid Etaee, Dr. Joshua Kindelan, Dr. Walter Lech, and Dr. Kimberly Mcfarland, dedicated vein experts you can rely on.
Book your consultation today at the clinic nearest you.